Many Americans have largely returned to a normal lifestyle they enjoyed before the COVID-19 pandemic began, but that doesn’t mean there still aren’t dangerous risks from infection. Scientists from the National Institute of Neurological Disorders and Stroke (NINDS) reveal in a recent study how the immune response triggered by the coronavirus may damage the brain.
NINDS researchers analyzed the brain changes in nine people who died suddenly after contracting COVID-19. They ranged in age from 24 to 73. They were chosen because they showed signs of blood vessel damage in the brain based on structural brain scans.
The study shows antibodies attacked the cells lining the brain’s blood vessels, which led to inflammation and damage. COVID-19 was not detected in the patients’ brains, suggesting the virus was not infecting the brain directly.
“Patients often develop neurological complications with COVID-18, but the underlying pathophysiological process is not well understood,” says Dr. Avindra Nath, study senior author and clinical director at NINDS, in a statement. “We had previously shown blood vessel damage and inflammation in patients’ brains at autopsy, but we didn’t understand the cause of the damage. I think in this paper we’ve gained important insight into the cascade of events.”
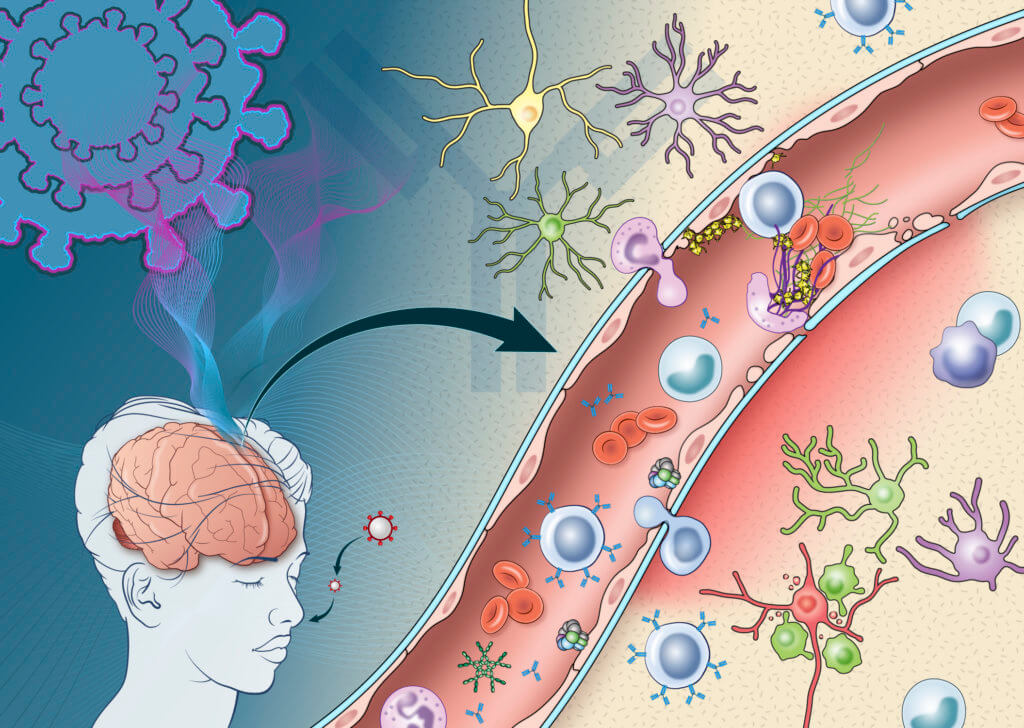
Antibodies produced due to COVID-19 may mistakenly target cells crucial to the blood-brain barrier. Scientists say there was damage to the endothelial cells in blood vessels in the brain, which can lead to leakage of proteins from the blood. Because of this, some COVID-19 patients suffer from bleeds, clots and stroke.
Researchers say, for the first time, they observed deposits of immune complexes — molecules formed when antibodies bind antigens — on the surface of endothelial cells in the patients’ brains. These immune complexes can damage tissue by triggering inflammation.
Dr. Nath and his team compared the nine brains to 10 others in the control group and looked at neuroinflammation and immune responses using immunohistochemistry, which uses antibodies to identify specific marker proteins in the tissues.
They “found evidence that damage to endothelial cells was likely due to an immune response — discovering deposits of immune complexes on the surface of the cells.” These findings suggest an antibody-mediated attack that activates endothelial cells. When these cells are activated, they express proteins called adhesion molecules that cause platelets to stick together. High levels of these molecules were found in endothelial cells in the samples of brain tissue.
“Activation of the endothelial cells brings platelets that stick to the blood vessel walls, causing clots to form and leakage to occur. At the same time the tight junction between the endothelial cells get disrupted causing them to leak,” explains Dr. Nath. “Once leakage occurs, immune cells such as macrophages may come to repair the damage, setting up inflammation. This, in turn, causes damage to neurons.”
Researchers believe their study may help treat long-term neurological symptoms stemming from COVID-19, including headaches, fatigue, loss of taste and smell, sleep problems and “brain fog.” Researchers believe had these nine patients survived, they would have developed long COVID.
“It is quite possible that this same immune response persists in Long COVID patients resulting in neuronal injury,” says Dr. Nath. “There could be a small indolent immune response that is continuing, which means that immune-modulating therapies might help these patients. So these findings have very important therapeutic implications.”
The study was published in the journal Brain.












Does this mean that everyone who has had Covid has a certain amount of Brain damage?